Study Links Long Covid to Increased Dementia Risk via Brain Damage

A groundbreaking study has uncovered a potential link between long Covid and an increased risk of developing dementia. Researchers in New York City analyzed data from over 80 individuals with long Covid, comparing them to healthy adults and those who had recovered fully from Covid-19. The findings suggest that long Covid may damage a critical brain structure known as the choroid plexus (CP), which plays a vital role in producing cerebrospinal fluid (CSF) and regulating brain inflammation. This discovery could reshape understanding of how the virus affects the nervous system long after initial infection.
The study, published in the journal *Alzheimer's and Dementia*, used blood tests and MRI scans to examine participants. It found that individuals with long Covid had a 10 percent larger CP compared to healthy controls. This enlargement was associated with biomarkers linked to Alzheimer's disease, the most common form of dementia. Researchers noted that the CP's role in waste clearance and immune support makes it a key player in neurological health. Damage to this structure could hinder brain function over time, potentially accelerating cognitive decline.

Long Covid, defined as symptoms lasting at least three months after infection, affects an estimated 20 million Americans. The condition often includes fatigue, brain fog, and shortness of breath—symptoms that are frequently dismissed or misdiagnosed. Despite growing awareness, the long-term consequences of the illness remain poorly understood. The study highlights a concerning possibility: that chronic inflammation from long Covid might lead to vascular remodeling in the CP, reducing CSF production and allowing waste to accumulate in the brain.
Researchers emphasized that the link between CP enlargement and Alzheimer's biomarkers is preliminary. Dr. Yulin Ge, a senior study author and professor at NYU Grossman School of Medicine, explained that the swelling in the CP could act as an early warning sign for future cognitive decline. The team observed that participants with larger CPs performed about two percent worse on cognitive tests, such as the Mini-Mental State Exam. These results suggest a potential pathway from long Covid to Alzheimer's-like symptoms, though more research is needed to confirm causation.
The study also revealed demographic differences among participants. Long Covid patients were, on average, younger (61 years old) than those in the other groups (72 years old). They were more likely to have higher body mass indexes, smoke, drink alcohol, and have preexisting conditions like high blood pressure and diabetes. These factors may compound the risk of neurological damage, though the study did not directly link them to CP changes.
Experts caution that the findings should not be interpreted as definitive proof of a direct cause-and-effect relationship. Dr. Thomas Wisniewski, director of the Center for Cognitive Neurology at NYU Langone Health, stated that the next step is to track participants over time to determine whether CP alterations predict long-term cognitive issues. He stressed the need for larger studies to clarify whether these changes are a cause or consequence of neurological symptoms.
The implications of this research are significant. With 7 million Americans aged 65 and older already living with Alzheimer's, and that number expected to nearly double by 2050, understanding risk factors is critical. The study adds to a growing body of evidence that long Covid may have lasting effects on the brain. However, researchers emphasize that public health efforts should focus on early intervention, monitoring, and further investigation rather than immediate conclusions.
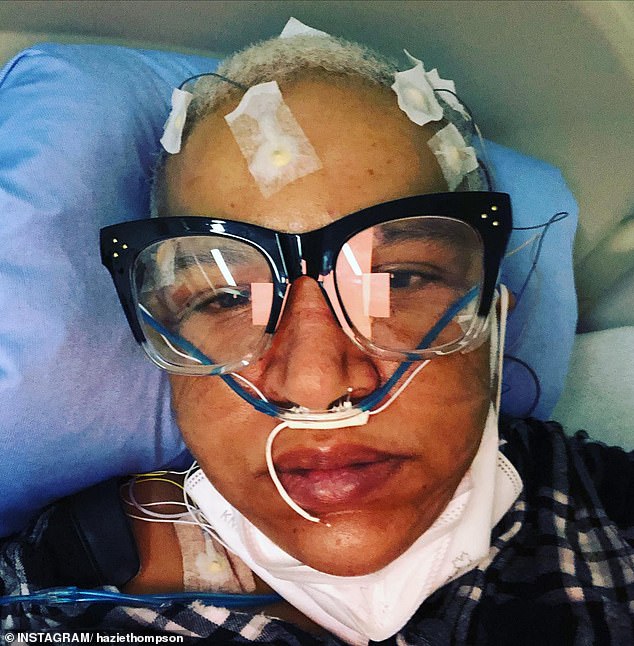
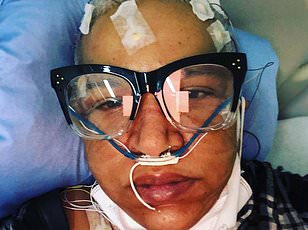
Patients like Tracey Thompson and Kirsty Huxter, who have lived with severe long Covid symptoms, underscore the urgency of these findings. Thompson described considering assisted suicide due to the severity of her condition, while Huxter was left bedbound for months. Their stories highlight the human toll of the illness and the need for better treatment strategies. Yet, the study does not yet provide answers for patients but instead sets the stage for future research into the neurological impacts of long Covid.
Public health officials and medical experts are advised to remain cautious in interpreting these results. While the study offers valuable insights, it is one piece of a larger puzzle. The limited access to long-term data on long Covid patients means that conclusions must be drawn carefully. However, the findings do reinforce the importance of monitoring individuals with long Covid for early signs of cognitive decline and ensuring they have access to supportive care.

In the coming years, further research will be essential to determine the full scope of long Covid's impact on brain health. For now, the study serves as a reminder that the pandemic's legacy extends beyond acute illness, potentially reshaping the trajectory of dementia and neurological disease for millions of people.
Photos




