Rising GP Consultations on Weight-Loss Medications Highlight NHS Strain Amid Private Access Surge, MPs Told
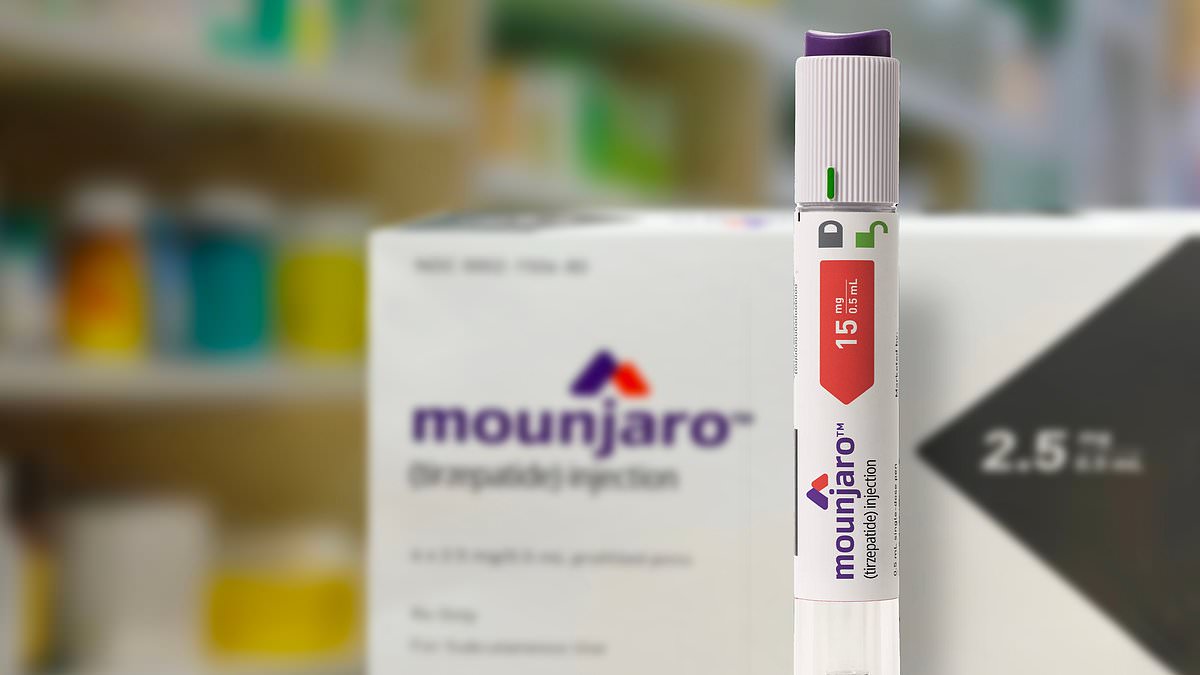
A growing number of general practice consultations are being devoted to discussions about Mounjaro and other weight-loss medications, according to a GP who raised the issue before a parliamentary committee. The statistic highlights an increasing trend where individuals are accessing these drugs through private means before presenting to the NHS with complications or adverse effects.
During a session of the Health and Social Care Select Committee on Wednesday, MPs were briefed on the rising number of patients seeking NHS care due to complications linked to these weight-loss jabs. Dr Munro Stewart, a GP Partner and vice-chair of the Royal College of General Practitioners, emphasized the surge in demand and the resulting burden on the NHS. He revealed that in November alone, over 263,000 prescriptions for Mounjaro were issued at a cost of £60 million to the NHS, indicating the scale of the challenge.
Dr Stewart further noted that around two million individuals are estimated to be using Mounjaro through private channels. He described the situation as increasingly concerning, with patients returning to the NHS for follow-up care after experiencing side effects or adverse interactions with other medications. He explained that he regularly receives letters from private prescribers regarding patients who have been given the drug outside of NHS oversight.
Dr Kath McCullough, a consultant in diabetes and endocrinology and obesity advisor to the Royal College of Physicians, echoed these concerns. She highlighted an uptick in emergency department visits linked to side effects from the entire class of weight-loss drugs. In a recent survey of GPs, it was found that one in 25 GP appointments is now primarily about Mounjaro or includes a discussion about the weight-loss jab. Additionally, some patients present with complications from interactions between the drug and other medications, such as contraception or hormone replacement therapy.
Dr McCullough warned that some private prescribers are not conducting thorough checks before dispensing these medications. She described practices that rely solely on patient self-reporting as 'dubious' and raised concerns about the lack of regulation in the private sector. She emphasized that healthcare workers should not assume that only obese or overweight individuals need these drugs, given the influence of online advertising that promotes the drugs without rigorous medical evaluation.
Both Dr Stewart and Dr McCullough stressed the importance of focusing on obesity prevention rather than relying on weight-loss medications as a primary solution. Dr Stewart warned of the potential over-medicalisation of obesity, noting that this could significantly strain NHS resources. He argued that prevention remains a cornerstone of effective healthcare, despite the role of these drugs in specific cases.
Dr McCullough added that the notion that obesity prevention is solely about diet and exercise is outdated. She called for a broader approach to tackling the issue, one that considers social, economic, and environmental factors.

The debate comes amid the announcement of a new NHS contract, which offers GPs a potential bonus of up to £3,000 per year for prescribing Mounjaro to eligible patients. Officials hope the financial incentive will encourage family doctors to speed up the rollout of the drug, which can help patients lose up to a fifth of their body weight in over a year. However, not all GP practices are currently prescribing the treatment despite having the authority to do so for eight months.
It is estimated that 2.4 million people in the UK are using these drugs, with at least two million paying around £200 per month for private prescriptions. NHS England has initiated a phased 12-year rollout of the once-weekly injection, prioritizing only 220,000 patients in the first three years. Currently, the drug is available on the NHS for severely obese individuals with a body mass index over 40 and complicating illnesses such as high blood pressure, obstructive sleep apnoea, cardiovascular disease, and type 2 diabetes.
Health Secretary Wes Streeting expressed optimism about the potential of weight-loss drugs to transform care for those in need. He emphasized that access should be determined by medical need, not financial capacity. He highlighted the issue of rogue prescribers outside the NHS offering unlicensed drugs that put patients at risk. Streeting noted that these measures are part of a larger public health strategy aimed at addressing the £11 billion annual burden that obesity places on the NHS and economy. He described the incentives for GPs as a step toward fairness in accessing obesity jabs, ensuring that those with the highest clinical need are prioritized.
The proposed bonuses for GPs could total up to £25 million annually, signaling a significant shift in how the NHS approaches obesity treatment. However, the controversy over the increasing use of weight-loss drugs in private and NHS settings continues to highlight the need for robust regulation, thorough medical evaluation, and a greater emphasis on prevention.
Photos



