New Research Warns: Omeprazole Linked to Mineral Depletion and Serious Health Risks

Every day, millions of Americans take a pill they trust to ease their heartburn and protect their esophagus. Omeprazole, sold under the brand name Prilosec, is a cornerstone of modern medicine. But what if this drug, so widely used for decades, is quietly damaging the body in ways its users never expected? Scientists in Brazil are sounding the alarm, revealing how this popular proton pump inhibitor (PPI) could be triggering a cascade of life-threatening side effects.

The research, conducted at the Federal University of São Paulo, offers a stark warning: omeprazole may be sapping the body of essential minerals, with consequences that ripple through blood health, bone strength, and immune function. The drug, designed to reduce stomach acid for short-term relief, is often taken for years, even decades, by millions. Yet its long-term use may be doing far more harm than good. How can a medication trusted to heal become a silent thief of vital nutrients?
To understand the danger, we need to look at what happens inside the body when omeprazole is taken. Stomach acid is not just a source of discomfort—it's a key player in absorbing minerals like iron, calcium, and copper. By suppressing this acid, PPIs can disrupt the body's ability to maintain these critical elements. In a 60-day study on rats, researchers found that omeprazole caused a shocking domino effect: copper levels in the liver plummeted, impairing iron absorption. At the same time, iron accumulated in organs instead of circulating in the blood, where it's needed to produce red blood cells. This double whammy could explain why long-term users of PPIs face higher risks of anemia and fractures.
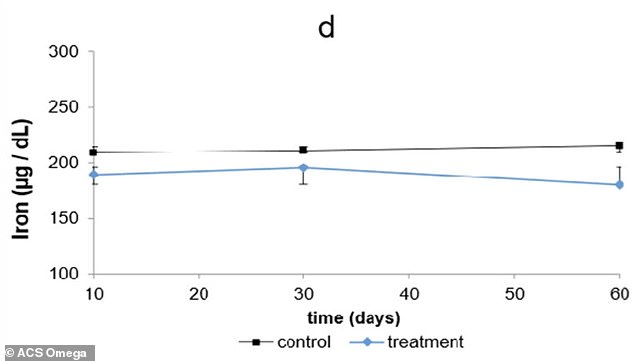
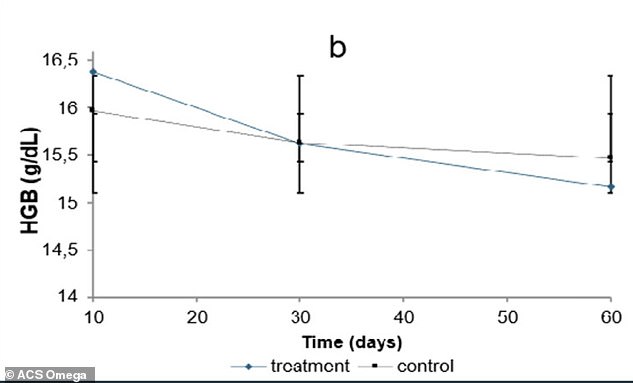
The findings paint a troubling picture. In the study, rats treated with omeprazole for 60 days showed significantly lower iron levels in their blood compared to a control group. Hemoglobin, the protein in red blood cells that carries oxygen, also dropped steadily. The consequences are dire. Anemia can leave people feeling exhausted, dizzy, and unable to think clearly. Without enough oxygen, the body's cells starve, and even simple tasks like climbing stairs become a struggle. Could this be happening to the millions of Americans who take Prilosec every day without knowing it?
The damage doesn't stop there. Calcium, the mineral that strengthens bones, was also affected. The study found that the body was pulling calcium from bones to maintain blood levels, a process that could lead to weakened skeletons over time. This explains the increased fracture risks seen in some long-term users. Imagine your bones becoming brittle like old paper—how would you feel if your body was quietly breaking down your own structure to keep you alive in the short term?
Even the immune system seems to react. The rats had elevated white blood cell counts, suggesting an inflammatory response. This might be the body's way of fighting off bacteria that thrive in the reduced stomach acid environment. After all, if the stomach is less acidic, harmful microbes have an easier time surviving and spreading. Is it possible that Prilosec's intended effect is also letting dangerous bacteria take root in places they shouldn't be?
Prilosec is among the top 10 most prescribed medications in the U.S., with over 45 million prescriptions written annually. Yet, the study's authors warn that these drugs are meant for short-term use only—typically four to eight weeks. Millions, however, take them indefinitely, often without medical supervision. What happens when a medication is used far beyond its intended purpose? The answer, according to this research, is a ticking time bomb of health risks.
Scientists caution that while the study was conducted on rats, the biological processes involved in mineral absorption are similar in humans. This raises urgent questions: Should patients who need long-term PPI therapy, such as those with Barrett's esophagus, be monitored more closely for mineral deficiencies? Can the risks be mitigated with regular blood tests and supplements? Experts say yes—but only if doctors and patients are aware of the dangers.
The implications are far-reaching. Communities reliant on these medications, from aging populations to those with chronic digestive issues, may be unknowingly facing a crisis of nutritional depletion. Public health officials and medical professionals must now grapple with a difficult question: How do we balance the benefits of these life-saving drugs with the risks of long-term use? The answer will require clear communication, regular monitoring, and a renewed focus on the invisible toll these medications may be taking on the body.
As more research emerges, one thing is clear: the drugs that help us today could be harming us tomorrow. The challenge now is to ensure that patients are not left in the dark, with their health compromised by a medication they trusted to heal.
Photos




