Columbia University Breakthrough: Lab-Grown Human Knee Offers New Hope for Osteoarthritis Patients

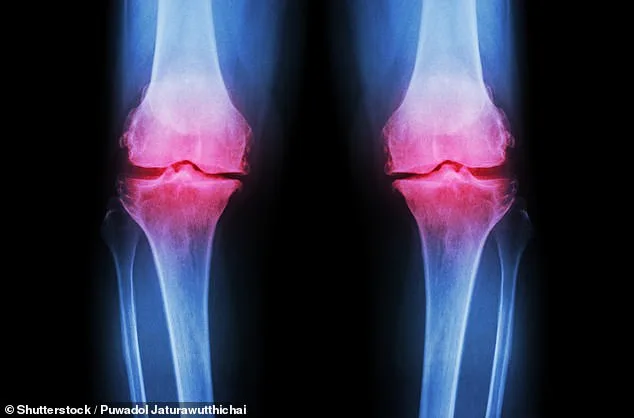
A groundbreaking advancement in treating osteoarthritis has emerged from Columbia University, where scientists have successfully grown a fully functional human knee in the lab. This innovation involves creating a 3D-printed scaffold using biodegradable materials, which is then seeded with bone and cartilage cells. Over the course of a year, these cells regenerate natural tissues while the scaffold dissolves, resulting in a complete lab-grown knee. Researchers believe this could be transplanted into patients, offering a permanent solution for those suffering from severe joint degradation. Osteoarthritis, which affects 32 million Americans—14 million specifically in the knees—is a leading cause of disability, with current treatments limited to pain management or invasive surgery. This new approach represents a potential paradigm shift in regenerative medicine, targeting the root cause rather than merely alleviating symptoms.
The prototype knees developed by Columbia's team have already been tested on cadavers, where they demonstrated the ability to bear weight and support movement. The next phase of research involves implanting these living joints into large animals, though the specific species remains undisclosed. If successful, human trials could follow within three years. Scientists emphasize that the lab-grown knees are designed to integrate with the body's vascular system, ensuring normal function post-transplantation. While the technology is currently focused on knee joints, researchers have not yet determined if it can be adapted for other affected areas, such as hips or foot joints. The project has received a $39 million grant from the Advanced Research Projects Agency for Health (ARPA-H), which funds cutting-edge therapies aimed at tissue regeneration.
Parallel efforts are underway at Duke University, where researchers have developed an injectable treatment that could stimulate cartilage and bone regrowth within joints. This injection, administered directly into affected areas, contains compounds designed to trigger tissue repair. In animal trials, the treatment restored joint tissue to near-normal levels and significantly reduced pain indicators. Dr. Benjamin Alam, who led the Duke team, described this as a critical step toward addressing the root cause of osteoarthritis rather than just managing its symptoms. The treatment is expected to enter first-in-human clinical trials in the coming years, though widespread availability may still be years away.
Meanwhile, scientists at the University of Colorado, Boulder, have introduced two novel therapies aimed at accelerating joint repair. One approach involves a single injection that recruits the body's own cells to regenerate damaged cartilage within weeks. These therapies, still in early testing, could complement existing treatments by offering faster and more localized healing. Together with Columbia's lab-grown knees and Duke's injectable solution, these innovations signal a transformative era for osteoarthritis care. If proven effective, they could reduce reliance on invasive surgeries and long-term pain management, improving quality of life for millions. Regulatory approval and clinical validation will be crucial as these treatments move closer to real-world application.
What if joint pain could be reversed without surgery? Researchers may be closer than ever to making that a reality. A groundbreaking study involving animal models with osteoarthritic joints has shown that targeted injections can restore joint health within four to eight weeks. In trials where the treatment addressed cartilage or bone defects, scientists observed "full regeneration and repair of the defect." These findings, published in a recent journal, have sparked excitement among medical professionals and patients alike.
The injections, administered directly into the joints, use a novel approach that harnesses the body's natural healing processes. Unlike traditional treatments that merely manage symptoms, this method aims to reverse damage. Dr. Elena Martinez, a lead researcher on the project, explained, "We're not just slowing the progression of osteoarthritis—we're actively repairing the tissue." The team is now preparing for human trials, which could begin in as little as 18 months. If successful, this could mark a paradigm shift in orthopedic care.
Funding for this research comes from ARPA-H, the Advanced Research Projects Agency for Health, part of the U.S. Department of Health and Human Services. The NITRO program, which backs the project, focuses on regenerative treatments for osteoarthritis. "Through ARPA-H, we're driving toward a future where people don't have to wake up in pain," said Alicia Jackson, ARPA-H director. "NITRO's progress helps damaged joints work again, slashes pain, or even eliminates it." The agency's support underscores the potential of this innovation to transform millions of lives.

Osteoarthritis is the most common form of arthritis globally, and its prevalence has surged in recent decades. Data from the World Health Organization shows a 132% increase in cases since 1990. Experts attribute this rise to aging populations, rising obesity rates, and socioeconomic disparities. Dr. Raj Patel, a rheumatologist at a leading U.S. hospital, warned, "We're seeing more patients than ever before. Traditional treatments aren't keeping up with the demand." With over 500 million people affected worldwide, the need for alternatives is urgent.
The new treatment could offer a lifeline to those facing joint replacement surgeries—a procedure that carries risks like infection and long recovery times. For many, the prospect of avoiding such interventions is a game-changer. "This isn't just about reducing pain," said patient advocate Maria Gonzalez, who has lived with severe osteoarthritis for years. "It's about regaining independence and quality of life." If human trials confirm the treatment's safety and efficacy, it could become a standard option within a decade.

Public health officials and medical experts are cautiously optimistic but emphasize the need for rigorous testing. "While the animal results are promising, we must ensure this works in humans," said Dr. Sarah Lin, a bioethicist at a major university. "We also need to address access issues—this treatment shouldn't be limited to wealthy individuals." With global health systems already strained by the pandemic, equitable distribution of any new therapy will be critical.
As research moves forward, the question remains: Can this breakthrough truly change the trajectory of osteoarthritis care? For now, the science suggests it's possible. The next step is proving it works in people—and making it available to those who need it most.
Photos




