Breakthrough in Male Contraception: Safe, Reversible Option Using JQ1 Drug

A groundbreaking development in reproductive health has emerged from a new study suggesting the possibility of a safe, reversible male contraceptive. Researchers are now exploring the potential of an existing drug, JQ1, which targets a specific protein involved in sperm production. This discovery marks a significant step forward in addressing the long-standing challenge of creating effective contraception for men, who currently have limited options compared to women. Dr. Paula Cohen, a genetics professor at Cornell University's College of Veterinary Medicine and lead author of the study, emphasized the importance of this research: "We're practically the only group that's pushing the idea that contraception targets in the testis are a feasible way to stop sperm production." The findings offer hope for a future where men can take on a more active role in family planning without enduring the side effects commonly associated with female contraceptives, such as weight gain, mood swings, and blood clots.
The research team focused on identifying a biological target that could temporarily halt fertility while preserving the body's ability to recover. For years, scientists struggled to find such a target because traditional approaches either risked permanent infertility or failed to prevent pregnancy entirely. The breakthrough came when researchers examined meiosis—the phase in sperm production where chromosomes pair up, exchange genetic material, and then separate into individual sperm cells. By targeting this specific stage, the team found a way to block fertility without harming stem cells, which remain intact and capable of restarting the process once the drug is discontinued.
In the study, male mice received daily injections of JQ1 for three weeks. The drug works by blocking a protein called BRDT, which is only active during sperm production. After treatment, the mice became infertile: their testicles shrank, sperm counts dropped dramatically, and testicular tissue revealed stalled development. Under microscopic examination, cells progressed to the point where they should have matured into sperm but then halted. Genetic sequencing confirmed that a normal "transcriptional burst" during meiosis had been silenced, effectively halting the process. This detailed analysis provided a roadmap for future male contraceptives, showing how a drug could safely interrupt fertility without causing permanent damage.
When the drug was discontinued and the mice were observed for six weeks, their bodies began to recover. Testicle size and sperm counts returned to normal levels, and the mice regained the ability to father offspring. However, the researchers noted lingering issues: the genetic crossover points where chromosomes exchange DNA had not fully recovered. While this suggests that full fertility might take longer to restore, it also highlights the potential for a reversible method. The study's authors stress that this approach avoids the hormonal changes associated with traditional contraceptives and could offer a non-invasive alternative for men.
Experts in reproductive health have cautiously welcomed the findings but emphasize the need for further research before human trials can begin. Dr. Emily Tran, a reproductive endocrinologist at the University of California, San Francisco, noted that while the results are promising, "long-term safety and efficacy in humans remain unproven." She added, "This is a critical step, but we must ensure that any future contraceptive doesn't carry unforeseen risks, especially for men who may be considering this as a long-term option." Public health advocates have also called for transparency in the development process, urging scientists to address concerns about accessibility and affordability once the technology advances.
The potential impact of this research extends beyond individual health choices. With nearly half of women currently using contraception—many of whom experience adverse side effects—a male contraceptive could help redistribute the burden of family planning. It may also empower couples to make more informed decisions about reproduction, reducing unintended pregnancies and improving overall public well-being. As scientists continue to refine the drug's mechanism and explore its long-term effects, the prospect of a safe, hormone-free, and reversible male contraceptive moves closer to reality, offering a transformative solution for reproductive health in the 21st century.

Some sperm still looked misshapen under the microscope, with bent flagella and abnormal heads, and certain gene programs related to sperm energy and movement remained disrupted. Those deeper measures took significantly longer to heal, about 30 weeks or seven months. Only then did those genetic crossovers, gene activity and sperm shape become indistinguishable from untreated mice. Even though some molecular and structural aspects of sperm took much longer to fully normalize, this delay did not translate into fertility problems or birth defects in offspring. The mice eventually healed completely and their babies were healthy. By comparing treated mice to untreated mice at every step — after treatment, at six weeks, at 30 weeks and in the next generation – they could see exactly what broke during drug treatment and whether it truly returned to normal.
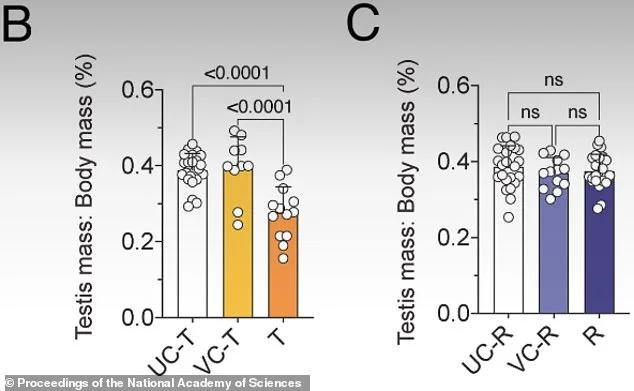
Figure L shows that after three weeks on JQ1, treated mice (T) showed a significant reduction in developing sperm cells compared to untreated (UC-T) and vehicle controls (VC-T). Figure M shows that six weeks after stopping the drug, developing sperm cells had returned to normal levels. Recovery mice (R) showed ratios comparable to untreated (UC-R) and vehicle (VC-R) controls. Most of those things did, though a few took longer. Eventually, they reported in the Proceedings of the National Academy of Sciences, everything returned to normal.

For decades, the search for a male birth control pill has been something of a scientific pipe dream. The biology is generally more difficult to crack. Women release one egg per month, a predictable cycle. Men produce hundreds of millions of sperm daily, around 1,500 every heartbeat. Shutting down this factory without killing libido, causing permanent infertility, or triggering nasty side effects turned out to be a much larger endeavor. After decades of starts and stalls with constant barriers to success, including painful injections, spikes in cholesterol, mood swings and unpredictability. A pill version never materialized and major pharmaceutical companies had abandoned the male contraceptive space in the 1990s altogether.
Unintended pregnancies account for nearly 44 percent of all pregnancies worldwide, and the burden has fallen almost entirely on women. Current male contraceptives are limited to condoms and vasectomies. Many men are wary of vasectomies, the only long-acting option available to men. While the procedure is technically reversible through a second surgery, reversal is expensive and not always successful. 'So we were really motivated to look for non-hormonal contraceptive targets in the testis, something that stops sperm production without affecting male libido and secondary sex characteristics,' Cohen said.
Recent advances in genetics and cell biology have opened new paths that did not exist twenty years ago. Instead of flooding the body with hormones, researchers are now targeting the sperm production process itself, finding precise molecular switches that exist only in the testis. While the drug is not ready for humans — it has significant side effects, including immune suppression, weight loss at higher doses, potential neurological effects, and broader toxicity concerns — it serves as a proof of concept; an ability to avoid using hormones at all.
Photos



