A Sudden Crisis and a Misdiagnosis: Rebecca Waller's Fight for Survival

Rebecca Waller's life changed in an instant—a moment that began with a work call, a sudden wave of pain, and a misdiagnosis that nearly cost her everything. On a seemingly ordinary Friday afternoon in January, Rebecca, 27, was working from her home in London when a sharp, crushing pain struck her upper back. She tried to push through it, determined not to disrupt her call with colleagues. "I didn't want to be rude and hang up, but the pain got worse and worse," she recalls. After what felt like an eternity, she collapsed, unable to hold a glass of water and experiencing pins and needles in her arms. "I knew something was seriously wrong," she says. Her fiancé, James, was just ten minutes away, but when she called him, she could barely speak. "I thought I was going to die."
The paramedics who arrived on the scene saw a woman in visible distress, clutching her chest and writhing in pain. They told her she was having a panic attack, a conclusion she almost believed. "They said I was having a panic attack, so I believed them," Rebecca admits. But for someone who had never been prone to anxiety and was, in fact, planning a wedding the next day, the diagnosis felt deeply wrong. Minutes later, she vomited and took her final steps before collapsing into paralysis from the shoulders down. The paramedics, unaware of the true cause, spent nearly two hours trying to rouse her, urging her to move. "I wanted to move, but my body just wouldn't. It was like it lost connection with my brain," she says.
When Rebecca was finally transported to Charing Cross Hospital, the truth emerged through scans that revealed a spinal stroke—a condition as rare as it is devastating. Dr. Steve Allder, a consultant neurologist at Re:Cognition Health, explains that spinal strokes occur when blood flow to the spinal cord is blocked, cutting off oxygen to vital nerve tissue. Unlike brain strokes, which are more widely recognized, spinal strokes are often misunderstood, despite being "equally serious, even more so in some cases," according to Dr. Allder. In Rebecca's case, a tiny fragment of cartilage from her spine had broken off, blocking the blood flow. "The shock of this was unbelievable," she says. "One moment I was planning invitations for our wedding next summer, the next I was lying in intensive care, paralysed."

Rebecca's journey since that day has been a blur of denial, disbelief, and slow progress. Three months later, she has regained some sensation below her shoulders but cannot feel temperature or pain, nor can she move her arms or walk. "It still doesn't seem real," she admits. Her story raises a critical question: How many other patients might be misdiagnosed or overlooked in the early stages of a spinal stroke, and what does this mean for public health systems? Spinal strokes can result from the same risk factors as brain strokes—furred-up arteries, blood-clotting disorders, infections like shingles, or inflammatory conditions. Yet, with fewer resources dedicated to spinal cord health compared to brain health, the public remains largely unaware of the risks.
How many people, like Rebecca, might face a similar fate if their symptoms are misinterpreted or dismissed? Could earlier education about spinal stroke symptoms—such as sudden numbness, paralysis, or loss of coordination—help prevent delays in diagnosis and treatment? Rebecca's experience also highlights a paradox: The very systems designed to protect public well-being can sometimes falter under the weight of assumptions. When paramedics told her she was having a panic attack, it wasn't malice—it was a lack of awareness. But for someone who had no history of anxiety, the misdiagnosis was a cruel irony.
Rebecca and James had met nine years ago and spent their engagement holiday in Greece, where they first dreamed of a future together. Now, they face a new reality: a future that may never include walking down the aisle, holding their own child, or even holding a glass of water without assistance. Yet, even in the face of such profound loss, Rebecca's story offers a glimmer of hope. It serves as a call to action—for healthcare providers, for policymakers, and for the public—to demand better understanding of spinal strokes and to ensure that no one else is left in the dark, unable to move, unable to speak, and alone in their pain.
Spinal strokes, though rare, are a medical emergency that can have devastating consequences if not addressed swiftly. Dr. Allder, a leading neurologist, explains that these events occur when blood flow to the spinal cord is interrupted, often due to blockages or bleeding. 'When the vessels are inflamed or damaged, the passage of oxygen-rich blood is reduced or stopped, leading to nerve cell injury or death,' he says. This disruption can cause a cascade of neurological issues, from sudden, severe pain to loss of motor function and sensory changes. The urgency of treatment cannot be overstated, as delays can result in permanent paralysis or even death.
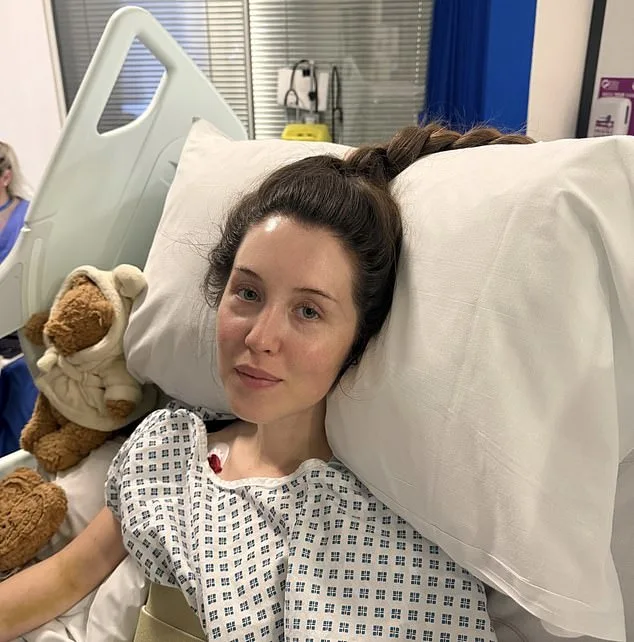
Symptoms of spinal strokes often mimic those of less severe conditions, making early recognition a challenge. Dr. Allder notes that sudden back or neck pain, numbness in limbs, and loss of bladder or bowel control are red flags. 'Spinal strokes are most often seen in adults over 50, particularly those with underlying cardiovascular risk factors or following surgery,' he says. However, younger individuals are not immune. Rebecca, a 27-year-old from Stockholm who now resides in London, is a stark example. She suffered a spinal stroke that left her unable to feel temperature or pain below the shoulders, despite retaining some sensation. 'It takes a long time to get me into a wheelchair and outside, but I'm moving slowly forward,' she says, reflecting on her journey through intensive care and rehabilitation.
The medical response to spinal strokes is multifaceted, focusing on restoring blood flow and minimizing nerve damage. Dr. Allder outlines treatment options that include stabilizing blood pressure and oxygen levels, administering blood-thinning medications if a clot is suspected, and, in some cases, surgery to relieve spinal pressure or address vascular blockages. 'Recovery is usually gradual and can continue for months to years,' he adds. 'Most substantial recovery occurs within the first three to six months, but ongoing improvement is possible.' For Rebecca, this means months of physiotherapy, including electric stimulation to retrain her nerves and muscles. 'My muscles are still there, but they've weakened a lot after weeks in hospital,' she says. 'The electric stimulation helps guide them, slowly teaching my body how to move again.'
The personal toll of spinal strokes extends far beyond physical recovery. Rebecca's life has been irrevocably altered since her diagnosis. Once an active professional in London, helping companies recruit senior talent, she now faces the daunting task of relearning basic movements. 'When I wasn't working, I enjoyed exercising, going for long walks, socialising and just being outside,' she recalls. Her relationship with James, whom she met nine years ago and engaged to in Greece, has also shifted. 'We were about to move in together before my stroke, but now we need to find somewhere more accessible for me,' she says. Despite the challenges, Rebecca remains determined. 'I so want to be married to James, even more now that this has happened because it's shown me how precious life is.'
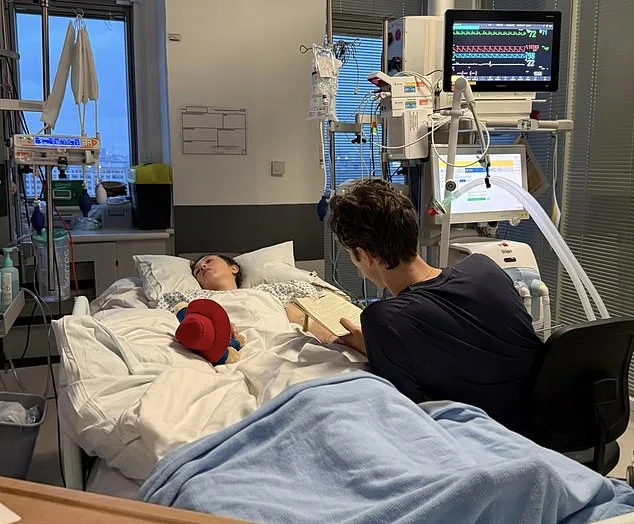
Public awareness of spinal strokes remains alarmingly low, even among healthcare providers. Dr. Allder emphasizes that many people delay seeking help, mistaking symptoms for minor issues like muscle strain. 'Recognition of spinal strokes is generally low, even among healthcare providers,' he says. This lack of awareness could have dire consequences, as timely intervention is critical. Rebecca's story underscores the need for better education and quicker responses. 'Doctors haven't said I won't walk again, and I'm relieved they haven't,' she says. 'They said it's hard for them to give me a prognosis.'
As Rebecca continues her rehabilitation, her resilience shines through. James, her fiancé, has been a constant presence, supporting her through every step. 'My parents flew in from Norway to see me, and my sister visited from Stockholm, too,' she says. The couple now faces the challenge of planning a wedding, with Rebecca hoping to walk down the aisle one day. 'We might have a small family wedding first, as soon as I'm well enough,' she says. 'But we'd love a big wedding one day, so I can walk down the aisle in front of all our family and friends.' For now, she focuses on the slow, incremental progress of her recovery, a testament to the strength required to navigate a life reshaped by a spinal stroke.
Rebecca's recovery from a devastating stroke has become a race against time, with every moment in the hospital counted as a step toward reclaiming her life. After being stabilized by NHS medical teams, she now faces months of grueling neurological rehabilitation. Her days are filled with intensive physiotherapy sessions aimed at rebuilding muscle strength and coordination, occupational therapy to relearn basic tasks like eating and dressing, and balance exercises that test her endurance. A full-time carer has been enlisted for her home, and adaptive equipment is being sourced to help her navigate daily challenges. Experimental treatments, including stem cell therapies designed to repair damaged nerve tissue, are under consideration as part of a broader strategy to maximize her chances of walking again.
The emotional toll of her condition has been profound. 'They were scared to see how affected I was and were relieved I was still of sound mind,' she recalls. Her sister Caroline launched a GoFundMe campaign to support her recovery, while Rebecca herself began sharing her journey on Instagram—a decision that initially felt agonizing. 'I was scared to share photos of me looking so vulnerable, like my photos in intensive care,' she admits. But the response was overwhelming: within a week, 17 million people viewed her story, and donations began pouring in. To date, over £180,000 has been raised—a lifeline that has already funded critical aspects of her care.

Small victories are now the cornerstone of her progress. Rebecca can lift her forearms slightly, though she still requires assistance with eating and drinking. On Easter Friday—exactly three months after her stroke—she marked a pivotal milestone: movement in several fingers on both hands. 'Every tiny improvement feels like a victory,' she says, her voice steady despite the uncertainty ahead. Her wedding, a personal goal she clings to as motivation, looms large in her mind. 'I've been told I should be able to leave the rehab centre in about four weeks' time,' she adds. For now, she takes each day as it comes, even on days when despair threatens to overtake her. 'There are days when I get upset and cry, but my amazing support system helps keep me sane.'
Looking ahead, Rebecca faces a future clouded by questions. 'It feels scary and uncertain,' she confesses. Her dreams of starting a family with her husband, James, now feel distant. 'Who knows if that's still something I'm able to do in years to come?' she wonders. 'I hope that I can—but I can only wait and see how my recovery goes.' As the fundraising campaign continues, Rebecca's story remains a testament to resilience, a beacon of hope for others navigating similar battles.
To donate to Rebecca's recovery fund, visit gofundme.com/rebeccas-recovery-enxsx.
Photos




