A Mother's Triumph: Overcoming IVF Struggles and NHS Barriers at 47

Jessica Peacock, 47, from Essex, stands in her living room cradling a baby monitor, her eyes glowing with the kind of joy that seems to defy time. At 46, she became a first-time mother after spending over £70,000 on IVF, a journey marked by four miscarriages, ten failed cycles, and a relentless pursuit of parenthood. "I was devastated when I found out we couldn't have children naturally," she recalls, her voice trembling slightly. "I didn't think about age because Ian and I met later in life. All I cared about was being happy and having a child." Her husband, Ian, 49, who already has two teenagers from a previous relationship, faced a cruel catch-22: NHS guidelines barred them from IVF funding because of his existing children, regardless of their age or living arrangements. "It's a postcode lottery with IVF," she says, her frustration palpable. "We were told we had to pay privately or never have a baby."
The couple's ordeal began years before their son Oliver was born. Jessica, a fertility mentor by trade, knew the science behind low egg reserves and endometriosis but had no shield against the emotional devastation that followed. "When I fell pregnant after the first round of IVF, I was over the moon," she says. "But when I miscarried, my dreams were shattered." The grief was visceral. She describes imagining her child's face, only to be struck by the cruel irony of a pregnancy lost before birth. After a manual vacuum procedure to remove remaining tissue, the couple endured three more miscarriages and seven additional IVF cycles in the UK. "We spent all our money trying," Jessica admits. "I was physically, mentally, and emotionally done."

Desperation led them abroad. In Spain, where IVF is available until age 51, they found a glimmer of hope. But even there, challenges loomed. A diagnosis of hydrosalpinx—where fallopian tubes fill with fluid—complicated matters further. "I was told I might never have a child," Jessica says. Yet, in a final act of defiance, they returned to the UK for one last attempt. A new clinic discovered a previously overlooked issue: Jessica's immune system was attacking embryos. With revised treatment and a focus on gut health, nutrition, and daily walks, she carried Oliver to term. "I was so scared," she recalls. "My anxiety was huge until 20 weeks. But I had a lovely pregnancy with no issues."
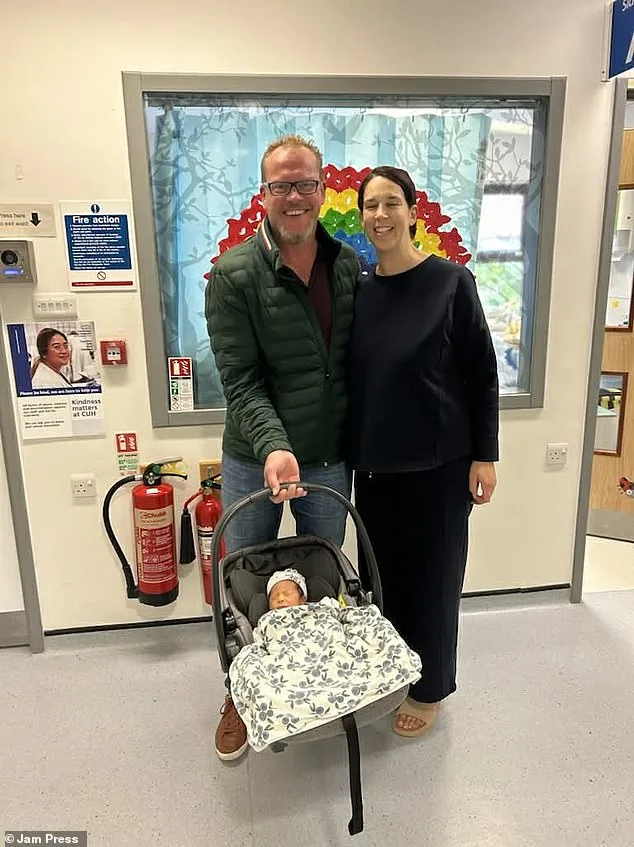
Now, with Oliver—now one—thriving in her arms, Jessica reflects on the toll of their journey. "I love being a new mum in my forties," she says, her voice steady. "We've traveled, partied, and now we have a family. I wouldn't change it for the world." Yet, the road ahead is uncertain. The couple is brooding over another child, though experts caution against the risks of advanced maternal age. Dr. Emily Hart, a reproductive endocrinologist, notes that while IVF success rates decline after 45, some women do achieve pregnancy with donor eggs and meticulous care. "It's not impossible," she says, "but it requires realistic expectations and support systems."
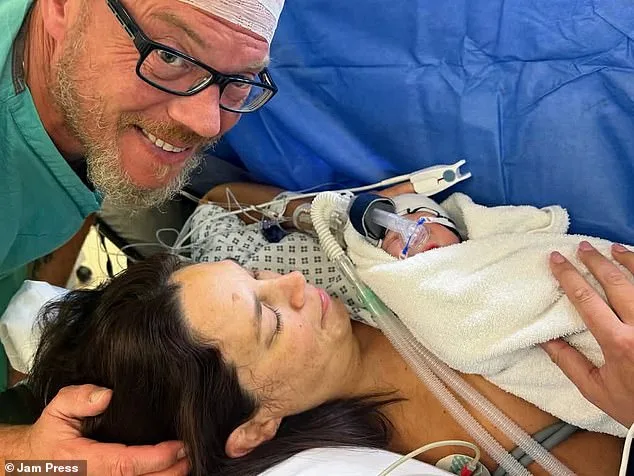
For Jessica, the past is a mosaic of heartbreak and resilience. She speaks of Oliver as her "miracle baby," a testament to love, science, and sheer willpower. Yet, even in victory, she acknowledges the cost: financial strain, physical toll, and the shadow of uncertainty. "I'm broody for another baby," she admits, though the path forward remains fraught with questions. As she gazes at Oliver, his laughter echoing through the room, one truth is clear: for Jessica Peacock, motherhood was never just about biology—it was a battle fought on every front, and a victory hard-won.
The Human Fertilisation and Embryology Authority (HFEA) has issued a stark warning about a growing crisis in UK fertility care, revealing that women seeking in vitro fertilisation (IVF) are now starting treatment at an average age of 35—the highest on record. This marks a six-year gap compared to the typical age of women giving birth naturally, a shift that experts say is dramatically reducing the success rates of IVF. "Every year that passes after 35, the chances of a successful pregnancy drop significantly," said Dr. Emily Hartley, a reproductive endocrinologist at London's Queen Charlotte's and Chelsea Hospital. "This isn't just a statistical concern—it's a human one."
The HFEA's report highlights a perfect storm of systemic failures. NHS fertility clinics, already stretched thin, have faced mounting pressure from pandemic-related delays and a backlog of appointments that has left many women waiting months for treatment. Sarah Thompson, 38, from Manchester, shared her frustration: "I was diagnosed with diminished ovarian reserve two years ago. I had to wait 10 months for my first consultation. By the time I started IVF, my options were already limited." Compounding these issues, the cost of private treatment—often exceeding £5,000 per cycle—has forced many to delay or abandon their plans altogether. "It's a Catch-22," said Thompson. "You can't afford to treat yourself until you're older, but the older you get, the less likely it is to work."
The consequences are stark. IVF success rates for women over 35 are roughly 20%—a figure that plummets further with each additional year. For those in their late 30s and 40s, the odds of a live birth drop to as low as 10%. This has created a cycle where delayed treatment leads to fewer chances of success, which in turn pushes more women into the private sector, further straining an already fragile system. "The NHS is not failing because of a lack of resources," argued Dr. Hartley. "It's failing because of a lack of prioritisation. Fertility care isn't just about helping people have children—it's about preventing long-term mental health crises, financial strain, and social isolation."

Meanwhile, the pandemic has left lasting scars. Lockdowns disrupted routine care, and many women postponed treatment out of fear of infection. "We saw a 40% drop in IVF cycles during 2020," said HFEA spokesperson James Carter. "Now, those delays are catching up." For some, the impact is irreversible. A recent study found that women who delayed treatment until after 38 were twice as likely to require donor eggs, a costly and emotionally taxing option.
The report has sparked calls for urgent reform. Advocacy groups are pushing for expanded NHS funding, shorter waiting times, and subsidies for private treatment. "This isn't just a medical issue—it's a moral one," said campaigner Priya Mehta, whose own journey through IVF ended in failure due to delayed care. "Every woman deserves the chance to build a family without being forced into a race against time." As the HFEA warns, the clock is ticking—and for many, it's already too late.
Photos




